Most of the general public in Barrie recognizes the word gingivitis, and thanks to some Listerine commercials in the 80’s, consider it a problem to be feared. We’ve written about gingivitis before, and in its most common form, it’s not a big deal in our eyes. The real gum disease problem is periodontitis.
This post is not intended to be an all-encompassing academic treatise on the pathphysiology of periodontitis (it’s a blog post, for goodness sakes), it is more meant to be a quick reference article for our Barrie-area patients to know what we have to say about it. For any periodontists (gum specialists) out there who happen to be reading this by accident, yes, we realize that periodontitis comes in many forms, and that it is all too simplistic to pigeonhole it all as one.
To define periodontitis, we will just say that it is inflammation in the tissues surrounding the tooth, causing continued loss of those supporting tissues. By supporting tissues of the teeth, we are referring to the superficial gum tissue, the collagen-based periodontal ligament that anchors the tooth, and the bone to which the teeth are anchored. We don’t look at these things in isolation.
If someone has lost supporting tissue from around the teeth, but does not show signs of progressively destructive inflammation, we do not consider this to be periodontitis. For example, recession of gums caused by hard toothbrush scrubbing is not what we’re talking about here.
There once was a time when gum health was not really considered by dentists, likely because tooth loss from dental caries (cavities) was the big problem of the day. When the mechanisms of cavities were clarified, and prevention quickly dropped the dental decay rate and severity, the dental community started to pay more attention to gum disease. The understanding was quite rudimentary: people who had gum disease probably weren’t brushing well enough, so surely the smelly bacteria-laden plaque that they were leaving in their mouths were able to roam free and destroy gum tissue. Improve one’s oral hygiene, and you would lower the amount of gum disease.
This turns out to be only partially true. How then, to explain the considerable number of people with poor oral hygiene and no gum disease, or those who have good oral hygiene and still have gum disease? Look at these shameful photos of receded gums from some sucker: (actually, these are photos taken of Dr. Wong’s own mouth. Yep, he’s got gum disease)…
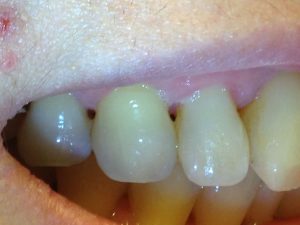
Something beyond simple oral hygiene/ bacterial levels must be at play. Indeed, things are more complicated:
1) bacteria- the mouth is one of the most bacteria-rich places in the body. There are not only large numbers of bacteria, but dozens of species that haven’t even been identified. Some of these bacteria are implicated in gum disease and some are not. It seems that certain bacteria are more damaging to gums than others in that they can serve as triggers for ongoing gum disease. (They don’t voraciously eat away at gum tissue, as you might imagine). Whether it is byproducts that they release, or molecules on their cell surfaces, their presence alerts the body that something nasty is present, and it had better get rid of it.
2) host susceptibility- this is the real answer: some people are more susceptible to gum disease than others, given the same bacteria. This is analogous to people who are at a higher risk of heart disease or diabetes, even though they live healthy lifestyles.
This largely boils down to an inherited genetic risk of gum disease, but can be affected by other general health conditions, such as stress, diabetes, or smoking. Dr. Wong blames it on dental school, but should probably also have chosen his parents more carefully.
So you need the right amounts and types of bacteria, and you need susceptibility. What happens next?
Once the bacteria trigger the patient’s own immune system response, there is an inflammatory reaction that is established in the gums. This typically chronic inflammation is what actually does the damage. In an effort to clear the body of bacteria or bacterial byproducts, the body’s own immune system ends up destroying its own gum, ligament, and bone tissues. Over time, less and less support remains for the tooth.
How is it detected?
Waiting until teeth get loose or gums develop abscesses is not a good approach. A medical history and a thorough dental examination, which includes detailed records of periodontal pockets, recessions, mobilities of teeth, furcations, tissue levels of attached and alveolar mucosa, and radiographs to determine bone levels should do the job. The bottom line: your Barrie dental office will tell you if something is up.
Great, but how do you treat it?
You simply have to change your genetic profile and reduce stress!
Kidding aside, we can only change so much. If you have been diagnosed with periodontitis, it is much better to manage it as early and as optimally as possible before things get out of hand.
This will always include some very thorough dental hygiene measures (cleaning the bacteria from the roots of teeth by physical scaling and root planing), possibly some adjuncts such as oral rinses, and other things that your dentist or hygienist may recommend for your particular condition. Sometimes we need to resort to antibiotics as well.
When things get more severe, you may require the services of a periodontist. These are trained dental specialists who deal with gum problems specifically. They may recommend surgery in addition to other interventions in order to maintain your teeth.
Left untreated, teeth will get looser and looser and the gums will recede, giving them the unsightly “long in the tooth” look. Food will trap in between the teeth more easily as spaces open up, and ultimately, teeth can be lost.
And the whole while, the process will probably be painless.
So, regular maintenance and examinations are crucial to early detection and treatment. Once treatment begins, continued vigilance is required to prevent any recurrences, as periodontitis is episodic. This will usually consist of hygiene visits more frequent than every six months, and occasional deeper cleanings.
We don’t yet know everything about periodontitis, or else we would be able to do much more. Still, there is value to making every possible effort to save your teeth, and proper prevention or management of periodontitis is an integral part of your overall care.
Questions? Contact us for a complete look at your teeth. We’d love to be your general dental office in Barrie.

